|
Onset and progression of manifestations of DC/TBD vary: at the mild end of the spectrum are those who have only minimal physical findings with normal bone marrow function, and at the severe end are those who have the diagnostic triad and early-onset BMF. Although most persons with DC/TBD have normal psychomotor development and normal neurologic function, significant developmental delay is present in both forms additional findings include cerebellar hypoplasia (Hoyeraal Hreidarsson syndrome) and bilateral exudative retinopathy and intracranial calcifications (Revesz syndrome and Coats plus syndrome). Other findings can include eye abnormalities (epiphora, blepharitis, sparse eyelashes, ectropion, entropion, trichiasis), taurodontism, liver disease, gastrointestinal telangiectasias, and avascular necrosis of the hips or shoulders. 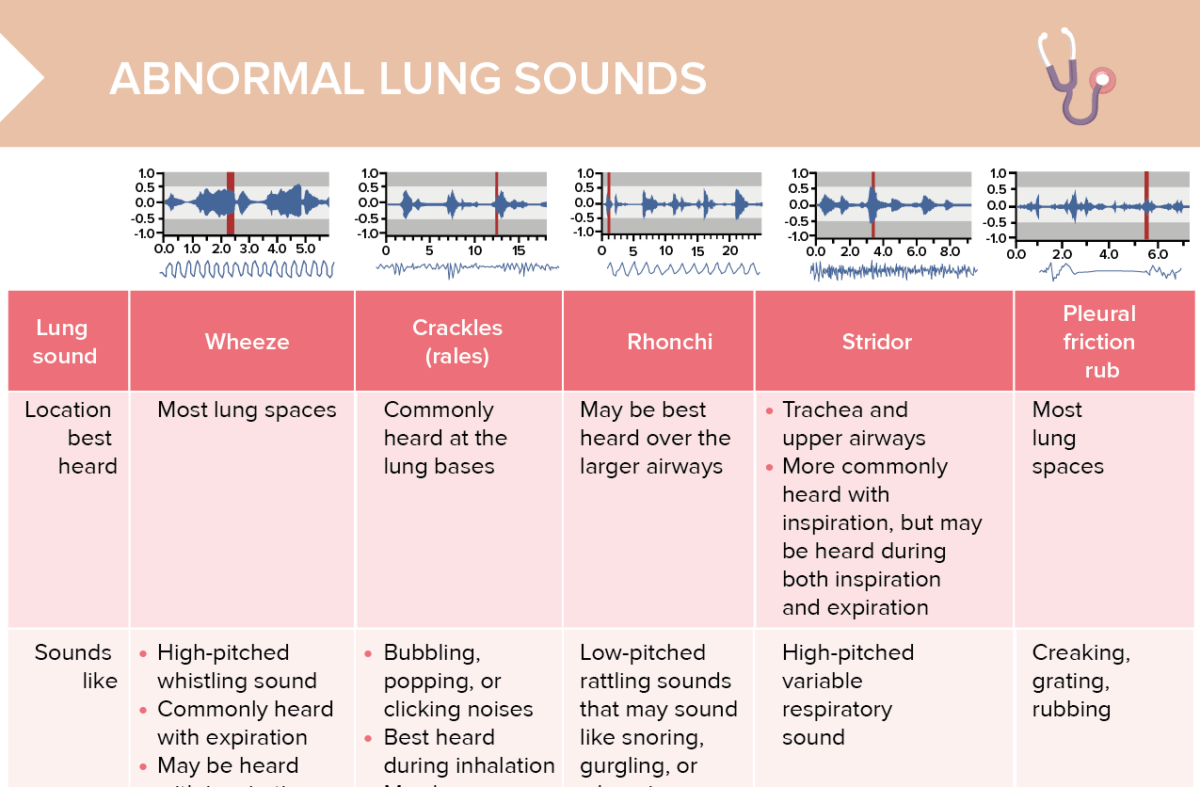
People with DC/TBD are at increased risk for progressive bone marrow failure (BMF), myelodysplastic syndrome or acute myelogenous leukemia, solid tumors (usually squamous cell carcinoma of the head/neck or anogenital cancer), and pulmonary fibrosis. Classic DC is characterized by a triad of dysplastic nails, lacy reticular pigmentation of the upper chest and/or neck, and oral leukoplakia, although this may not be present in all individuals. The phenotypic spectrum of telomere biology disorders is broad and includes individuals with classic dyskeratosis congenita (DC) as well as those with very short telomeres and an isolated physical finding. In one review, 50% of affected individuals had the full brain-lung-thyroid syndrome, 30% had involvement of brain and thyroid only, and 13% had isolated chorea only.ĭyskeratosis congenita and related telomere biology disorders (DC/TBD) are caused by impaired telomere maintenance resulting in short or very short telomeres. The risk for thyroid cancer is unknown and may not be increased. Abnormal lung sounds that include crackles (formerly called rales), stridor, wheezes (formerly called rhonchi), pleural friction rub, and stridor. Thyroid dysfunction, the result of dysembryogenesis, can present as congenital hypothyroidism or compensated hypothyroidism. The risk for pulmonary carcinoma is increased in young adults with an NKX2-1-related disorder. Pulmonary disease, the second most common manifestation, can include respiratory distress syndrome in neonates, interstitial lung disease in young children, and pulmonary fibrosis in older persons. Chorea generally begins in early infancy or about age one year (most commonly) or in late childhood or adolescence, and progresses into the second decade after which it remains static or (rarely) remits. Childhood-onset chorea, the hallmark of NKX2-1-related disorders, may or may not be associated with respiratory distress syndrome or congenital hypothyroidism. NKX2-1-related disorders range from benign hereditary chorea (BHC) to choreoathetosis, congenital hypothyroidism, and neonatal respiratory distress (also known as brain-lung-thyroid syndrome).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
